Case Reports
Case 6 : Mucinous Cystadenoma
Scripted by : Dr Kalpesh KhatalEdited by : Dr Sangeeta Jain, MD, Vridhi Fertility Centre, Vardhaman hospital, Ambala City
Contributed by : Dr Anirudh Badade
Introduction:
An ovarian cyst is a sac filled with liquid or semiliquid material that arises in an ovary. The number of diagnoses of ovarian cysts has increased with the widespread implementation of regular physical examinations and ultrasonographic technology. The discovery of an ovarian cyst causes considerable anxiety in women owing to fears of malignancy, but the vast majority of ovarian cysts are benign. These cysts can develop in females at any stage of life, from the neonatal period to postmenopause. Most ovarian cysts, however, occur during infancy and adolescence, which are hormonally active periods of development. Most are functional in nature and resolve with minimal treatment. However, ovarian cysts can herald an underlying malignant process or, possibly, distract the clinician from a more dangerous condition, such as ectopic pregnancy, ovarian torsion, or appendicitis.
Case report:
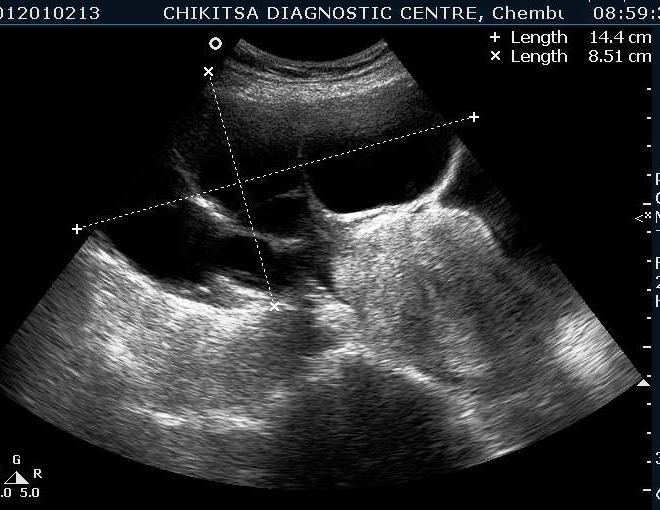
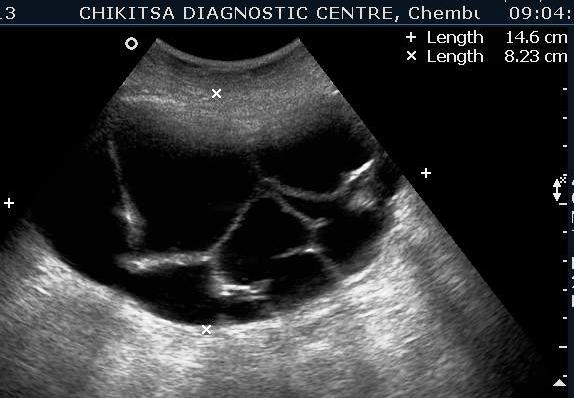
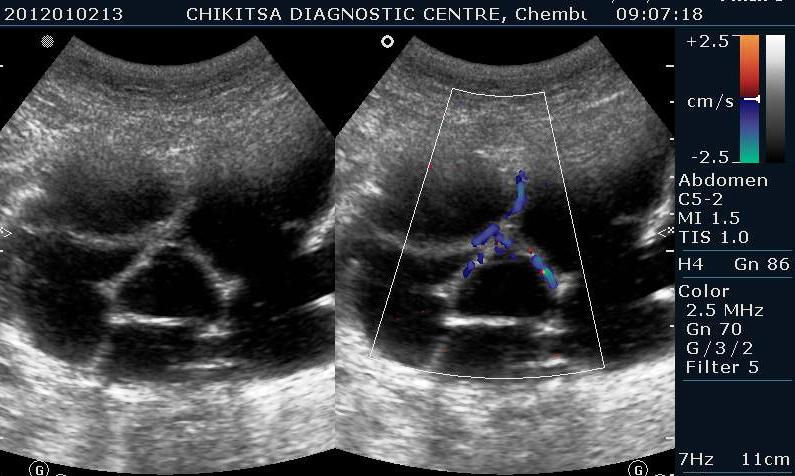
A 35 year old female was referred to our centre by a gynaecologist with gradually increasing distension abdomen & discomfort ,with pressure downwards. She had two alive children , both delivered normally & one early abortion , now tubectomised for 5 years.She had normal regular periods with cycle 3-5/25-35 days. No history of dysmenorrhoea.No history of any chronic medical illness. On ultrasound abdominally, one large mass of 15 cm x 10 cm with multiple septations was seen. On colour flow, vascularity was noted in the septal walls. No papillary projections seen in the mass.No solid areas seen in the mass.Uterus & right ovary were found to be normal. Diagnosis of left benign ovarian tumour ? mucinous cystadenoma was made which was confirmed on HPE after left ovariotomy .
DISCUSSION :-
Ovarian tumors include: 1. Epithelial tumors (65-75%) - serous or mucinous cystadenoma/carcinoma, clear cell carcinoma, Brenner tumor 2. Germ cell tumors (15%) - dysgerminoma, embryonal cell cancer, choriocarcinoma, teratoma 3. Sex-chord-stromal tumors (5-10%) - granulosa cell tumor, thecoma, fibroma 4. Metastatic tumors (10%) - uterine, stomach, colon, breast, lymphoma. Mucinous cystadenomas make up 15-20% of all ovarian tumors. They often become very large and can extend up into the abdomen. Pseudomyxoma peritonei can result if the tumor ruptures and spills its contents into the abdomen. These tumors are usually evaluated using ultrasound, CT scan, or MRI. Findings on imaging studies are nonspecific. These ovarian tumors are usually multi-septated, cystic masses with thin walls. They also contain varying amounts of solid tissue which consists of proliferating stromal tissue, papillae, or malignant tumor cells. Mucinous cystadenomas are divided into three categories: benign, borderline, and malignant. Survival is largely dependent on the histology of the tumor, with a 10 year survival rate of 100% for benign tumors, 60% for borderline tumors, and only 34% for the malignant subtype. There is some difference in ages of the peak incidence for the different subtypes with considerable overlap as described below. In general, benign tumors tend to present earlier, while malignant tumors are often seen later in life.
ULTRASOUND FINDINGS:
Multiple thin septae are present and low levels echoes due to mucoid material present in the dependant portions of the mass. In mucinous Cystadenomas, individual locules may vary in imaging appearance due to difference in degree of hemorrhage and protein content. That's the differentiating point between serous and mucinous. Smooth inner wall structures are more reliable characteristics in predicting benignity. Presence of solid components and lesion without measurable wall thickness and demonstrable inner wall structure suggested malignancy. The difference in chemical components and difference in viscosity is responsible for sonographic echogenicity.
Identification of papillary projections on an imaging study is important because they are the single best predictor of the epithelial character of a neoplasm and may correlate with the aggressiveness of the tumor.
Absence of ascitis favoured benign lesions and its presence meant more chances of the lesion being malignant.
Unilocular tumours less than 10 cm in diameter and without papillary formations had a low probability of malignancy - irrespective of the woman's age. This finding does not correlate with the findings of the present study.
Benign tumors are bilateral in 5-10% of cases. Borderline mucinous cystadenomas make up about 10% of mucinous ovarian neoplasms and are bilateral in 10% of cases.Malignant mucinous cystadenoms are rare, and encompass 10% of mucinous ovarian tumors and 5-10% of primary malignant ovarian neoplasms overall. They are bilateral in 15-30% of cases and have a peak incidence between 40-70 years of age.
Cancer antigen 125 (CA-125) :
- CA-125 is unreliable in differentiating benign from malignant ovarian masses in premenopausal women because of the increased rate of false positives and reduced specificity.
- CA-125 is primarily a marker for epithelial ovarian carcinoma and is only raised in 50% of early-stage disease.
- When serum CA-125 levels are raised, serial monitoring of CA-125 may be helpful, as rapidly rising levels are more likely to be associated with malignancy than high levels which remain static.
- Elevated in over 90% of patients with advanced ovarian carcinoma and in 50% of patients with early-stage ovarian disease.
- CA-125 is not specific for ovarian cancer and may be elevated in a number of other malignancies, menstruation, endometriosis, pregnancy, benign ovarian tumours and pelvic inflammatory disease.
- The main use of CA-125 is in assessing response over time to treatment for malignancy.
- CA-125 does not need to be done in premenopausal women who have had an ultrasound diagnosis of a simple ovarian cyst made.
Risk of Malignancy Index (RMI) : cut-off level of 200 to indicate malignancy
- There are different risk of malignancy scores which can be used to assess an ovarian mass
- The RMI I is the most effective for women with suspected ovarian cancer. This is also recommended by the National Institute for Health and Clinical Excellence (NICE) guideline on ovarian cancer.[5] It should not be used for premenopausal women though.
- RMI I combines three presurgical features: serum CA-125 (CA-125); menopausal status (M); and ultrasound score (U).
- The RMI is a product of the ultrasound scan score, the menopausal status and the serum CA-125 level (IU/mL) as follows: RMI = U x M x CA-125.
- The ultrasound result is scored 1 point for each of the following characteristics: multilocular cysts, solid areas, metastases, ascites and bilateral lesions. U = 0 (for an ultrasound score of 0), U = 1 (for an ultrasound score of 1), U = 3 (for an ultrasound score of 2-5).
- The menopausal status is scored as 1 = premenopausal and 3 = postmenopausal.
- Serum CA-125 is measured in IU/mL.
Acknowledgment:- We take immense pleasure in thanking Dr.Anirudh Badade for his able guidance and useful suggestions.
References
1) Turkyilmaz E, Korucuoglu U, Kutlusoy F, et al (March 2009). "Recurrent mucinous cystadenoma: a laparoscopic approach". Arch. Gynecol. Obstet. 279 (3): 387-9. doi:10.1007/s00404-008-0718-0. PMID 18584185
2) Ozgun MT, Turkyilmaz C: A giant ovarian mucinous cystadenoma in an adolescent: a case report. Arch Med Sci 2009, 5(2):281-283.
3) Yenicesu GI, Cetin M, Arici S: A huge ovarian mucinous cystadenoma complicating pregnancy: a case report. Cumhuriyet Med J 2009, 31:174-177
4) Grainger RG, Allison DJ. Imaging in Gynaecology. In: Whitehouse GH, Wright CH (eds). Grainger and Allison's Diagnostic Radiology. A Textbook of Medical Imaging. 4th Ed. 2004 Churchill Livingstone, 2215-21.
5) Sturgeon CM, Lai LC, Duffy MJ; Serum tumour markers: how to order and interpret them. BMJ. 2009 Sep 22;339:b3527. doi: 10.1136/bmj.b3527.
6) Ovarian cancer, NICE Clinical Guideline (April 2011); The recognition and initial management of ovarian cancer
7) Obeidat BR, Amarin ZO, Latimer JA, et al; Risk of malignancy index in the preoperative evaluation of pelvic masses. Int J Gynaecol Obstet. 2004 Jun;85(3):255-8. [abstract]
